October 5, 2021

Healthcare’s “Tech-tonic” Shift to Digitization and Virtualization
Since the iPhone’s legendary 2007 launch, healthcare gurus have predicted a “tech-tonic” shift to digital and virtual care modalities. That hasn’t happened. Industry incumbents have stalled the type of tech-led disruptive change that has transformed the transportation, hospitality, publishing and numerous other industries.
Given the healthcare industry’s entrenched commitment to status-quo business models and slow pace of change, each new year in healthcare almost always resembles the previous year. Predictions haven’t been terribly useful. Bold forecasts rarely materialize. COVID-19’s disruptive impact on consumer behaviors and healthcare delivery changes everything. The pandemic has accelerated healthcare’s transformation toward consumerism and new care delivery models.
New York Yankee great and part-time philosopher, Yogi Berra, reportedly observed, “Predictions are difficult, especially about the future.” Yogi has it right for almost every industry except healthcare. It’s impossible for incumbents to fight gravity forever.
Tech-driven disruption, however, is coming to healthcare. It will manifest through Payment, Platforming, and Personalization. These “3 Ps” will drive the industry’s application of digitalization and virtualization within health system business models.
This “tech-tonic” shift will make healthcare delivery more efficient, personalized and engaging. It will create enormous value by delivering better health outcomes consistently at lower costs with great consumer experience. Healthcare will never be the same.
The 3 Ps Driving System Transformation
Fueled by advances in AI, digitization, and virtualization, the 3 Ps shape how companies reconfigure business models and practices to engage consumers, enhance their convenience, energize employees, increase productivity, and grow market share.
These forces are entering the healthcare marketplace at scale. The following recent transactions incorporate these powerful technological and organizational capabilities into powerful business platforms that exemplify how healthcare transformation is unfolding in real time.
- Teledoc’s acquisition of Livongo
- Grand Rounds’ acquisition of Doctors on Demand
- Transcarent’s recapitalization and repositioning
- Amazon’s nationwide launch of its Amazon Care platform
These new tech-enabled business models are reinventing the healthcare customer experience and redefining consumer expectations. Service models are decentralizing, moving into the home, establishing 24/7 access, and optimizing virtual care delivery. These new care modalities challenge asset-heavy legacy business models and fragmented status quo service delivery.
Healthcare transformation will not happen overnight. It cannot fully happen until payment incentivizes desired outcomes (such as holistic care, prevention, health promotion, lower costs, better customer experience, etc.). At the same time, value-creating transformation is relentlessly reshaping healthcare delivery through new buying and selling behaviors getting traction within the healthcare marketplace. With that as background, let’s dive into the 3 Ps.
Payment
America won’t change the way it delivers healthcare until it changes the way it pays for healthcare. Current fee-for-service payment models incentivize transactional care delivery that is fragmented, duplicative, administratively complex, and wasteful. Worst of all, status-quo healthcare practices generate suboptimal care outcomes. [1]
Transformational payment models, such as full-risk bundles for episodic care and capitation for population health, align payment incentives with desired cost and quality outcomes. For example, Medicare partners with commercial health insurance companies to offer portable and personalized health insurance policies through its Medicare Advantage (MA) program. Under MA, health plans “own” their members’ healthcare risk, which gives them incentives to keep their members healthy by providing timely, appropriate and cost-effective care whenever necessary.
MA plans market actively to consumers to win their business. This has translated into expanded service offerings to lure new members. These can include zero premiums, gym memberships, dental care and full prescription drug coverage. Consequently, consumers make value-based purchasing decisions and the “fitter” companies will gain market share.
As full-risk contracting expands into the employer marketplace, the outdated link between employment and health insurance provision will wither. Workers will carry their health insurance with them as they transition to new employment.
Continuity of health insurance coverage will improve health outcomes. As health insurance products become more portable, consumers assume more control for their healthcare decision-making. Increased consumer engagement will accelerate price transparency, increase preventive care and shift routine care delivery to lower-cost, higher-convenience venues.
This isn’t speculative. Today, companies like Transcarent, Amazon, and others are enhancing the capabilities of healthcare consumers to make smarter healthcare purchasing decisions through “smart” technologies. Consumer-friendly applications enable consumers to overcome access and cost barriers. As they make more and better healthcare purchasing decisions, consumers are redefining the industry’s supply-demand dynamics from the bottom up.
Platforming
As proffered in a July 2020 commentary, synchronizing business and clinical operations through integrated and connected platforms makes healthcare better in meaningful ways every day. Integrating business and clinical workflows with more effective workforce strategy improves care outcomes, increases care delivery efficiency, enhances employee morale, and increases patient satisfaction. More broadly, platforming is a powerful organizing concept for managing complex organizations within digitizing marketplaces.
As digital exchanges (think Uber) facilitate better transactions for buyers and sellers, service suppliers are developing integrated platforms of connected capabilities (see chart). All companies have inputs and outputs. Great companies organize their owned, partnered, and contracted activities to deliver superior offerings to customers at competitive prices. Competition for customers drives innovation and organizational redesign.
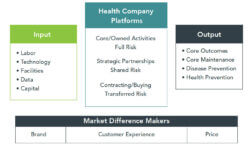
Organizing internal processes to optimize performance is essential to market success. Platform companies create value by seamlessly connecting their capabilities into a unified offering that engages customers on their terms. Unlike typical health systems, platforming health companies focus on outputs, not singular ownership and production control.
To thrive in customer-oriented markets, health systems must develop operating platforms to deliver better healthcare services at lower prices with great customer service. These will include “plug and play” strategic partnerships for essential services (e.g., urgent care) and enhanced digital connectivity with healthcare consumers.
Additionally, platforming health companies will make more effective resource allocation decisions by employing enhanced monitoring of employee activities to inform high-powered cost accounting systems. They will optimize adoption of human/ machine collaboration to reduce worker burnout, increase organizational efficiency/effectiveness, and facilitate ongoing customer engagement.
In essence, platformed health companies will succeed by delivering better outcomes at lower prices with great customer service. They will make healthcare better.
Personalization
The shared pandemic experience will have lasting impact in the ways people live, work, play, and manage their health. It will fundamentally alter healthcare consumption. Once the paradigm for healthcare service delivery, the one-size-fits-all approach is becoming obsolete.

Healthcare companies that tailor service provision to individual needs and preferences will achieve competitive advantage in the post-COVID marketplace. For example, the authors expect that FICO-like “health scores” for individual members will emerge to support underwriting decisions for aggregated groups and suggest proactive interventions for minimizing hospitalizations.
Already underway before COVID, the decentralization of care delivery and the adoption of virtual-care modalities accelerated during the pandemic. This includes a massive expansion of telehealth visits [2] as well as expanded provision of hospital-based services in the home [3] and usage of healthcare apps. [4]
In the evolving post-COVID healthcare marketplace, healthcare service providers must accommodate “benefit-plan-of-one” concepts in designing their business models. Platform companies must position themselves precisely to personalize service provision.
Healthcare’s conventional wisdom that “all healthcare is local” [5] is showing its age. Advances in AI, digitization and virtualization are increasingly personalizing healthcare access and service delivery. During the 2020s, healthcare will apply new technologies to do more than customize service delivery to increase convenience and accommodate customer preference.
Health systems also will incorporate individualized genotype and phenotype data to tailor individualized treatment and lifestyle regimens that will dramatically improve health outcomes, enhance well-being, and extend longevity. By the decade’s end, healthcare as we know it today will no longer exist.
Conclusion: Healthcare’s “Tech-Tonic” Shift Changes Everything
In the same way that shifting tectonic plates create earthquakes that permanently reconfigure landscapes, American society’s adaptive responses to the COVID-19 pandemic are permanently reconfiguring U.S. healthcare. The pandemic has revealed unacceptable fragmentation, access barriers, supply-chain vulnerabilities, and inequities embedded within U.S. healthcare.
Digitization and virtualization are disruptive forces pushing the healthcare industry toward value-based care delivery and consumerism. Americans no longer accept pre-COVID healthcare service levels. Historically, health systems have benefited from a defensive strategic orientation. [6] That approach will not work in the post-COVID marketplace. Health systems must be strategically proactive and embrace consumerism, risk-based payment and value-based care delivery.
Relative to other industries, healthcare has experienced less disruption and consequently lagged in technology adoption. Given these realities, healthcare will disproportionately experience post-COVID changes in a society-wide reconfiguration of workplace dynamics, service delivery, and consumer engagement.
Enlightened health systems will embrace payment reform, platforming and personalization to gain market share as the healthcare industry transitions and transforms. Healthcare’s future belongs to the bold and adaptive. As philosopher Yogi Berra might observe, “healthcare’s future just ain’t like it used to be.”
Sources
- William H. Shrank, M. D. (2019, October 15). Waste in the US Health Care System. JAMA. https://jamanetwork.com/journals/jama/article-abstract/2752664
- Koonin LM, Hoots B, Tsang CA, et al. Trends in the Use of Telehealth During the Emergence of the COVID-19 Pandemic —
United States, January–March 2020. MMWR Morb Mortal Wkly Rep 2020;69:1595–1599. DOI: http://dx.doi.org/10.15585/mmwr.mm6943a3. - Weiner, S. (2020, September 29). Interest in hospital-at-home programs explodes during COVID-19. AAMC.
https://www.aamc.org/news-insights/interest-hospital-home-programs-explodes-during-covid-19. - Natanson, E. (2020, July 23). Healthcare Apps: A Boon, Today And Tomorrow. Forbes.
https://www.forbes.com/sites/eladnatanson/2020/07/21/healthcare-apps-a-boon-today-and-tomorrow/. - The Clinton Foundation, C. (2017, August 9). Healthcare is Local. Medium. https://stories.clintonfoundation.org/healthcare-is-local-bcc165cc22eb.
- Lee, T. H., & Porter, M. E. (2015, September 14). The Strategy That Will Fix Health Care. Harvard Business Review. https://hbr.org/2013/10/the-strategy-that-will-fix-health-care.





