September 2, 2020

Achieving Data Aggregation at Scale: How Health Companies Will Adapt to the Age of Liquid Data
In Healthcare’s Age of Liquid Data, we explored why the healthcare industry must move aggressively to make healthcare data extremely connected. We identified three steps to make this happen – the industry must aggregate data, curate data and use the data to engage consumers in a personalized manner to harness the power of the interconnected data.
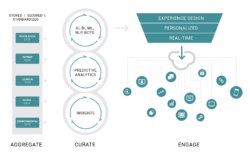
The transformation of healthcare will be data driven. Payers, health systems and other providers that embrace robust data and analytics and extreme interoperability can dramatically enhance their capacity to engage patients, support clinicians, enhance efficiencies, improve revenues, expand services and individualize the prediction, prevention, diagnosis and treatment of illness and disease.
Other industries have already reinvented themselves by developing platforms that combine in-person service with digital technologies. Think of banking, which was once a bureaucratic, brick-and-mortar enterprise, but today offers highly efficient and personalized services at the customer’s convenience.

Consider advanced data-driven organizations like Amazon, Google and Facebook. On the surface, they provide an array of services, devices and products. Fundamentally, however, they are in the business of collecting, curating and leveraging data. This gives them the capacity to understand and engage customers, improve processes, predict demand, develop new products and services, and study and enter new markets.
Healthcare is on the brink of a similar evolutionary leap. The technology for managing and utilizing healthcare data is already widely available and improving quickly. Now, new rulings by the Center for Medicare and Medicaid Services (CMS) and the Office of the National Coordinator for Health Information Technology (ONC) have expanded patient data access to providers, payers, third-party vendors and patients themselves. This will turbocharge data sharing, care coordination and consumerism while leading to an explosion of new products and services.
To compete effectively in this age of liquid data, traditional healthcare organizations will need to step up their technological capabilities and adopt a new mindset. That starts with developing the systems and capacity to aggregate, store, standardize and protect massive data sets.
5 Capabilities That Enable Aggregation
Healthcare has long been rich in claims data, patient information and clinical data. Leading organizations are already tapping into alternative data streams, including societal, demographic and environmental data, consumer and marketing data and genetic and population health data. The volume of available healthcare data is unprecedented.

Some of these data streams occur during normal workflow, others can be captured via monitoring devices, wearables, and technology platforms (like telemedicine) or purchased from proprietary sources. All data is valuable. It is a mistake to treat “irrelevant” data as exhaust. Data-focused companies compulsively collect and store all data, knowing that it might prove useful some day for unanticipated reasons.
As the volume of data expands exponentially, however, healthcare organizations must collect that information systematically and securely while enabling its accessibility. This requires developing robust capabilities in the following areas.
- Consolidation: Most healthcare organizations still use their existing transactional and operational systems for data storage, rather than using a separate data warehouse. This reinforces siloed approaches, and makes it difficult and more time consuming to access data, compare data sets and run reports. In an industry that increasingly competes on value, efficiency, innovation and service, all functions must have access to a single source of truth. Comparing data across functions, such as clinical and claims, can lead to game-changing insights and improved approaches to care delivery and revenue generation.
- Storage: Only a few years ago, it was necessary to build costly data centers to store massive data sets. Today, any organization – from the largest retailer to the smallest startup – can access third-party cloud storage platforms cheaply. Major vendors include Google’s GCP, Amazon’s AWS, and Microsoft’s Azure. Each platform has different strengths, weaknesses, features and services. Cloud platforms enable healthcare organizations to take an evolutionary leap in data management. Not only does the cloud free up significant financial resources, but it also facilitates easier access, cross-functional sharing and flexibility in application.
- Protection: Healthcare organizations need to protect their data. Health Insurance Portability and Accountability Act (HIPAA) compliance is sacrosanct, and patients are extremely sensitive about personal data security. Healthcare executives may resist proposals to store data externally due to fears of being hacked. In truth, few healthcare organizations come remotely close to the internal security capabilities that the three dominant cloud storage providers offer. When breaches occur, it’s not typically due to the platform itself. It’s usually the implementation and configuration of clients into these large platforms (which are usually done by third-party firms) where errors occur and breaches may follow. That’s why it’s imperative to select the right third party / partner that has the right expertise and experience.
- Standardization: Raw data incorporates multiple terms, languages and fields. Master data management brings IT and operational users together to give raw data uniformity and consistency, making it accessible and actionable across functions, platforms and tools. Organizations must develop a consistent way of mapping out and normalizing their data sets to enhance collaboration and insight generation.
- Access: Organizations also must systematically inventory their data sets to map all the data streams at their disposal. This data catalog helps users locate the data they are seeking in real time while assuring that data is right for their needs. This dramatically increases the speed and efficiency of data extraction while enhancing quality and utility.
It’s important to also acknowledge the exact of business healthcare organizations. The industry has a tendency to build and maintain services, functions and expertise in-house. Few organizations outside big tech, however, have the internal talent and know-how to design, implement and run data aggregation and storage processes.
Even when systems are in place, it’s critical to occasionally get expert audits to evaluate system performance and suggest upgrades or new approaches. Tools and best practices change all the time.
As CFOs evaluate the investments needed, they may be hesitant to spend money on data infrastructure, processes and outside services. However, those investments are often offset by the speed, efficiency and power of the insights they deliver, making such investments less expensive.
Takeaway: Enhanced Insights, Processes and Applications
The COVID-19 pandemic shone a harsh light on American healthcare’s urgent need for data interoperability. Lack of access to data hampered the ability to pinpoint hotspots, identify symptoms, perform contact tracing at scale, protect at-risk populations, source and distribute vital medical supplies, predict outbreaks, and optimize clinical treatments.
This data access/sharing problem has long plagued the healthcare system as a whole, driving up costs while hindering efficiencies, coordination and care quality. Yet the pandemic has also accelerated the digital transformation of the industry. After years of slow-walking new technologies and digital processes, health systems and payers are now rapidly migrating care delivery to virtual platforms and embracing data analytics and artificial intelligence. There is no going back.
With a solid infrastructure for data aggregation, organizations are better able to draw robust insights and make informed decisions and predictions. As healthcare becomes more dynamic, consumer-focused and value-based, this capacity can help the organization innovate, evolve and thrive.
Co-author
 Scott Rowe is the Chief Information Officer for Conifer Health Solutions, overseeing strategic technology initiatives for Conifer Health and driving technology innovations that enhance Conifer Health’s RCM capabilities. As CIO, Scott helps clients transform healthcare financial and revenue cycle processes through innovations in Artificial Intelligence, Applied Data Sciences and Digital Integration. Previously he served Conifer as VP and CIO of the Revenue Cycle Management business, and in various other leadership roles since the company formed in 2008. With more than 15 years of healthcare industry experience, Scott has seen first-hand how hospitals and health systems embrace technology to support nearly every aspect of care delivery. Scott earned a Bachelor of Business Administration in Management Information Systems from Baylor University and a Master of Business Administration with concentration in Finance from Auburn University.
Scott Rowe is the Chief Information Officer for Conifer Health Solutions, overseeing strategic technology initiatives for Conifer Health and driving technology innovations that enhance Conifer Health’s RCM capabilities. As CIO, Scott helps clients transform healthcare financial and revenue cycle processes through innovations in Artificial Intelligence, Applied Data Sciences and Digital Integration. Previously he served Conifer as VP and CIO of the Revenue Cycle Management business, and in various other leadership roles since the company formed in 2008. With more than 15 years of healthcare industry experience, Scott has seen first-hand how hospitals and health systems embrace technology to support nearly every aspect of care delivery. Scott earned a Bachelor of Business Administration in Management Information Systems from Baylor University and a Master of Business Administration with concentration in Finance from Auburn University.






