March 24, 2026
If We Can Eliminate Tuberculosis, Should We?
How Change Management Tools Could Help Us Address This Horrific Disease and Other Curable Ones Like It
What if we could eliminate history’s deadliest illness? I recently finished John Green’s New York Times Bestseller, “Everything is Tuberculosis.” As a public health enthusiast, I found the history of tuberculosis (TB) fascinating, but it was Green’s moral argument for eliminating TB that really stuck with me.
Throughout the story, he recounts the injustice of how active TB is in areas where treatments aren’t available (i.e., low-resource countries) and the treatments are abundant where the disease isn’t (i.e., high-resource countries like the U.S.). Annually, TB still kills over 1 million people, and in 2024, it claimed 1.23 million lives. Green claims, “We could choose to live in a world where no one dies of TB … we choose not to.”
Describing how societies could eliminate the disease, he lists a few key factors:
- Long-term, large-scale investments by wealthy countries to strengthen the health systems of poorer countries;
- Investments in new treatments;
- Better addressing drivers of health (poverty, inadequate housing, poor sanitation and working conditions, long hours, inadequate food), which he sees as the true cause of continued TB spread, as well as active disease and death.
Thanks to antibiotics, TB is curable. But it’s also a bacterium, so it evolves and, over time, becomes resistant to treatments. As pharmaceutical companies develop new cures, new drugs are cost-prohibitive for lower-resource countries. Green states, “Millions of lives can be saved in the next decade if we pressure governments and institutions to invest in research and the global effort to provide curative therapy.” He concludes the book, stating, “We are the cause. But we can also be the cure.”
While his argument is deeply compelling, it left me with one nagging question: “What would have to happen for his vision of no one dying from TB to become our reality?”
Admittedly, I struggled with the “how to” in this case, as I couldn’t see a pathway to achieve his vision that would be attractive to all parties involved in the complex and interconnected web of healthcare, governmental, and pharmaceutical stakeholders. It sounds great, but at first I doubted how it could actually be accomplished.
The more I thought about it, the more it became clear that two of The Christensen Institute’s theories offered a pathway to make Green’s vision a reality: not only for tuberculosis, but for other curable diseases and public health woes alike. These are 1) The Tools of Cooperation and 2) Business Model Theory.
Approaching the Problem: How Leaders and Drug Makers Could Collaborate to Spur Change
Last night, as I talked to my husband about the book, our conversation focused on how to solve the TB problem without the U.S.’s participation in the WHO, and with the current administration’s decisions to eliminate USAID (a move experts estimate could lead to an additional 10.7 million TB cases and 2.2 million more deaths over the next five years).
How can the world eliminate TB without the U.S. government at the table, or at least without it playing a very large role? First, my mind went to Christensen’s Theory of the Tools of Cooperation.
In brief, the Tools of Cooperation states that to guide effective change, leaders must understand where their stakeholders fall on two dimensions: organizational or societal goals and how outcomes are achieved (i.e., what inputs lead to what outputs). These two dimensions are plotted on the Agreement Matrix, shown below.
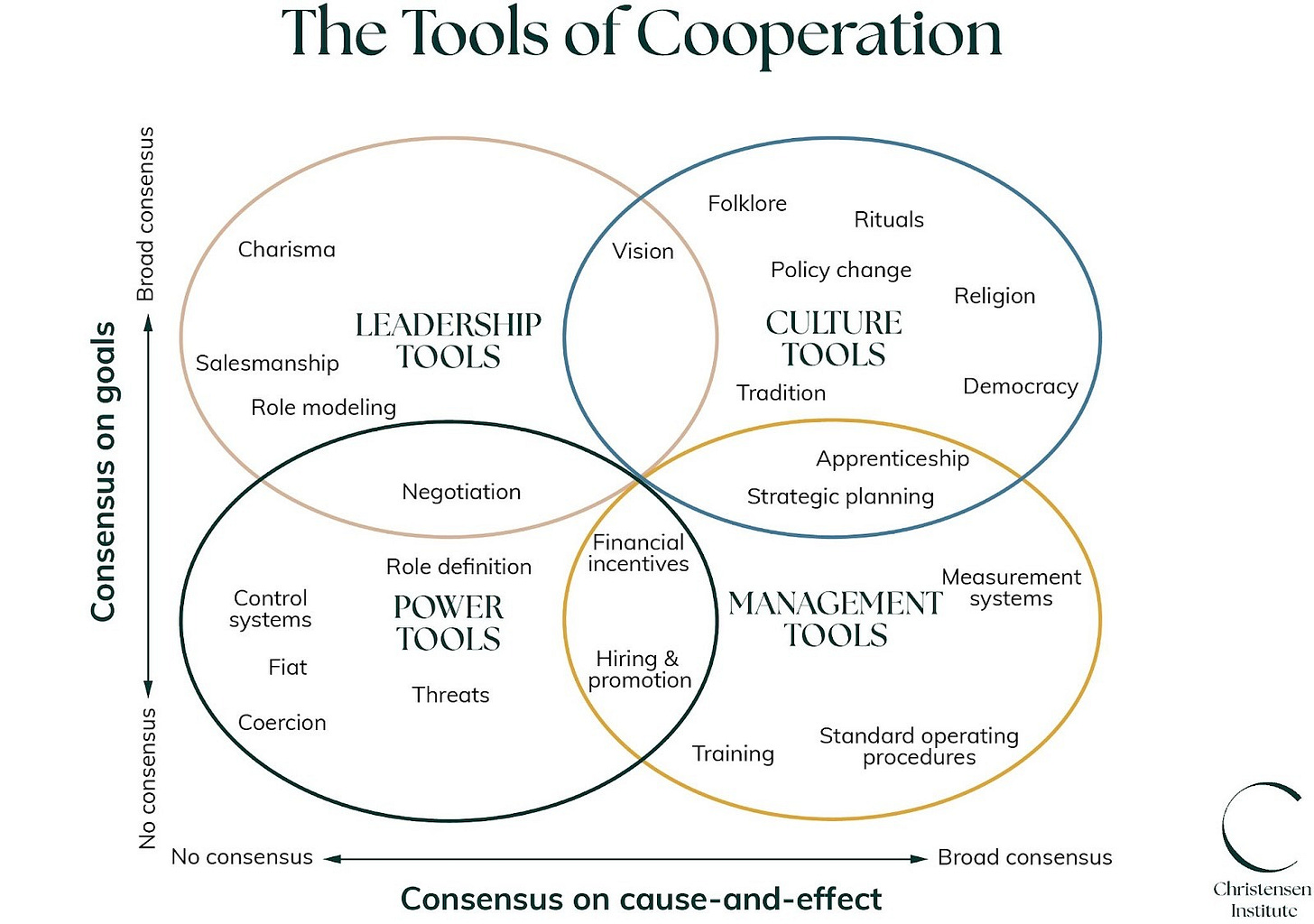
Once leaders identify their stakeholders’ consensus on goals and the pathways to achieve outcomes, leaders can leverage the most effective tools for the situation. The boundaries are directional, not rigid, and they help leaders match the change management tool to the situation their stakeholders are in, in order to drive effective change.
Putting ourselves in the shoes of lower-resource countries that bear the burden of higher TB disease and death, the critical questions to answer to determine the best-fit approach for change management are as follows:
- Which stakeholders are critical to solving the problem of high rates of active TB, associated illness and death?
- Where do those stakeholders fall in consensus on a goal?
- Where do those stakeholders fall in consensus on the pathway to achieve goals?
In this example, stakeholders would include the government, healthcare workers, the population of the focal country, and the drug maker who sells the most effective TB drug (currently, that drug is Janssen’s bedaquiline, which is owned by Johnson & Johnson). For the sake of this argument, let’s say the government of a highly impacted country is leading the charge for change.
Collectively, these stakeholders probably fall on the right-hand side of the X-axis, with a fair amount of agreement on how to solve the TB problem. Governments, health care workers, and populations in countries most affected by TB, as well as the drug makers themselves, likely believe more affordable drugs are one of the most effective pathways for a cure.
The agreement breaks down on the Y-axis. While the former group of stakeholders believes the goal of curing TB in their country is worthwhile, drug makers don’t seem to align. This is likely not because they’re bad people, but because agreeing with that goal would threaten the profit formula their company has been built to expect (more on that in a minute). So, we’d conclude that there is limited agreement on the goal, meaning stakeholders fall into the lower quadrants of goal alignment.
This assessment of stakeholders’ X- and Y-axis placement indicates that both financial incentives and measurement systems would be effective levers to address the problem of widespread, curable TB that is currently not effectively treated.
Determining which incentives and measures would be most effective to drive change leads us to the second theory that’s applicable in this situation: Business Model Theory.
Developing a Solution: Compelling Financial Incentives and Measures of Success (i.e., Priorities)
 One thing Green highlights in his book is the flaw of cost-effectiveness. Specifically, he focuses on its inhumanity, in that we shouldn’t put a price on saving someone’s life. If we can save them, we should. In public health and health care, the concept of a treatment’s cost-effectiveness is a core measure of success. Admittedly, as someone trained in public health and the importance of cost-effectiveness analyses, Green’s argument was hard to hear. But, from a human perspective, it’s also incredibly hard to disagree with him.
One thing Green highlights in his book is the flaw of cost-effectiveness. Specifically, he focuses on its inhumanity, in that we shouldn’t put a price on saving someone’s life. If we can save them, we should. In public health and health care, the concept of a treatment’s cost-effectiveness is a core measure of success. Admittedly, as someone trained in public health and the importance of cost-effectiveness analyses, Green’s argument was hard to hear. But, from a human perspective, it’s also incredibly hard to disagree with him.
Since cost-effectiveness is the prevailing measure leaders use to evaluate whether a treatment should be paid for or invested in, and the most effective antibiotics for TB are incredibly expensive, many in low-resource countries go without effective treatment. Instead, they receive medications that used to work for TB, but to which many strains of TB now have resistance.
As Christensen lays out in Business Model Theory, an organization’s priorities determine what it says “yes” to and what it says “no” to. As a result, some drug makers are saying “no” to providing antibiotics to low-resource countries with high TB burdens because those countries can’t afford the list price of their drugs. What gets measured gets managed, and what gets managed gets done. If we want to change what gets done, we’d have to change what gets measured.
Thinking about which incentives and measures would lead drug makers, and specifically Janssen, to agree to support the goal of curing TB in low-resource countries raises two questions:
- What could a different, but equally attractive, profit formula for drug makers look like?
- How could one change the cost-effectiveness calculation in order to save more lives and also preserve profits for drug makers?
Let’s start with the first question. To incentivize drug makers to sell TB drugs at a lower price point that middle- and low-income countries could afford, drug makers and affected governments could enter a profit-sharing agreement. Effectively, drug makers would trade smaller returns in the short run for larger returns over longer periods of time. This would require selling the drugs at a price point that made the investment in both TB treatment and prophylactic use cost-effective in the short-run (i.e., making it cost-effective for governments in countries with high TB burdens).
In exchange for affordable antibiotics to treat multi-drug-resistant TB (MDR-TB), countries could provide drug makers with a percentage of the increase in their annual GDP resulting from reduced disease burden and increased productivity. Effectively, lower TB rates function as a productivity stimulus. However, the agreement must maintain an attractive profit formula — even if it’s over the long-term — for drug makers, or they won’t opt in.
This could be a win-win set-up, allowing governments to treat TB, people to survive, countries to thrive, and drug makers to still achieve their desired margin. When countries have lower TB rates, more healthy children and working-age adults emerge, leading to higher education levels and greater productivity, in turn driving stronger GDP growth. Additionally, while this could be a near-term solution to increase the availability of TB drugs where they are most critically needed, it will also be interesting to watch how AI changes the equation.
AI could be a critical factor influencing the answer to the second question above. If AI exponentially speeds up drug development, the entire calculation of how pharmaceutical companies can gain a return on their research investment will shift, and drug prices could plummet.
A Viable Pathway Toward Green’s Desired Future
At the core of Green’s argument is an indictment of our morality.
He’s right that for a better future for all, we need to focus on the injustice and inhumanity of unnecessary death — death that occurs on a massive scale — and commit ourselves to changing it. In thinking about how to achieve change, though, we can’t ignore the structural realities of our current state, including deeply entrenched business models and dispersed but interconnected stakeholders. These factors aren’t easy to change or address. But the recommendations from the Tools of Cooperation and the necessity of new business model priorities highlight that change is feasible.
The pathway for change starts with understanding 1) which stakeholders need to be aligned for a solution to occur and how much they agree on goals and pathways to achieve them, and 2) what set of financial incentives and measures of success will spur drug makers to sell TB antibiotics at an affordable price, while not threatening their profit formula required to survive.
Eliminating TB and other curable diseases is within reach if we tap into both our desire to do what’s most humane and our understanding of what drives companies and governments to remain viable.





