September 16, 2020

What Pandemic? Investors Love Hotspotting 2.0
Key Takeaways
- Investors expressed confidence in Oak Street Health’s model for caring for high-cost, low-income patients by sending its shares soaring 90% on the first day of trading after an IPO.
- Oak Street Health uses a high-touch, primary care business model to take on full financial risk for almost all of its patients.
- Oak Street offer comprehensive primary care for high-cost Medicare and Medicaid patients. They use an enhanced version of the “hotspotting” model pioneered in Camden, N.J.
- Unlike the Camden model, these practices not only coordinate care, they help patients meet their basic needs for food, housing, clothing and social support.
- Their business plan calls for generating profits by reducing preventable hospitalizations and improving patients’ overall health status.
- Unless the government reverses course on social policy, their financial success will be very difficult to achieve.
In the summer of 2018, Yvonne Giddens, now 57, began treatment at the Oak Street Health clinic on Chicago’s impoverished West Side, carrying a bagful of medications. Two weeks earlier, she’d suffered three small strokes that left her hospitalized for four days. The hospital physician and discharge nurse said her blurry vision would clear up in a few weeks. It hadn’t.
Dr. Henish Bhansali, her new primary care physician, reviewed her prescriptions. They included blood sugar control pills for diabetes; four pain medications for her “fiery” leg pains and a bad back from a workplace injury she suffered when 23 years old; and an anti-seizure drug.
“He said he was going to fix everything,” she recalled when I first interviewed her five months later. “He said by June of next year, he would have me off all those pain drugs and get my blood sugar down.”
Oak Street Health is part of the growing group of start-up companies deploying intensive primary care to reduce spending on the 5% of patients – people like Giddens – who account for half of all healthcare spending. Oak Street focuses exclusively on Medicare patients, which covers seniors and the disabled. Founded in 2012, the rapidly growing firm operates 54 centers in 8 states and has assumed financial risk for 80,000 lives.
In early August, Oak Street Health raised $328 million through an initial public stock offering to further its expansion plans. Its stock price surged 90% on the first day of trading, an expression of investor confidence in its model for improving the lives – and thus lowering healthcare costs – for the people for whom its already assumed full financial risk.

Start-ups like Oak Street provide intensive primary and coordinated care for complex patients. Other firms in the space include IoraHealth (48 locations in 7 states); Landmark Health (in-home primary care in 14 states), ChenMed (59 locations in 9 states), Anthem’s CareMore (16 locations in 9 states and the District of Columbia), Absolute Care (4 locations in 3 states), and CityBlock in New York City. They collectively serve over 700,000 patients, a number that is growing rapidly.
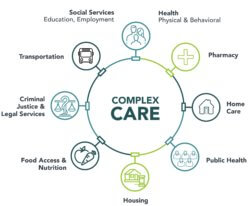
Their approaches differ in their particulars but follow common themes. They deploy care teams that include community outreach workers, care coordinators, social workers, in-house pharmacists and behavioral health specialists. They collaborate with community social service providers to help meet patients’ immediate need for food, transportation, and, upon occasion, housing – what healthcare policy analysts call the social determinants of health.
Their innovative care programs include a focus on prevention, especially of diabetes, which is surging among the nation’s poor due to rising obesity and the absence of affordable, nutritious food in low-income neighborhoods. They look for ways to provide emotional support for people who are under the constant stress of living at or near poverty, often in isolation.
Their clinics sometimes double as social spaces, offering bingo, cooking classes or simply a place to drop in and grab a cup of coffee. “We don’t have a social determinants of health strategy,” Dr. Griffin Myers, a co-founder of Oak Street Health and its medical director said. “We are a social determinants of health strategy.”
Why the Poor Need More Healthcare
Compelling observations about contemporary life in America drive these primary-care business models. Among advanced industrial countries, the U.S. is the least generous when it comes to providing income, housing, food and social support for its less fortunate citizens. It pays a hefty price for that neglect in the form of higher healthcare costs. As a group, low-wage workers and the poor have far more health problems than people of greater means, and they are far more likely to wind up as high-cost patients in public programs.
The assumption by firms like Oak Street Health is that by delivering better care coordination and crucial social support, they can lower overall health spending on these patients. They’re looking to make money in the process. Most of these venture capital-backed firms are taking on substantial financial risk by accepting capitated payments from Medicare Advantage insurers and Medicaid managed care organizations.
But their business strategies leave a number of crucial questions unanswered. Many high-cost patients with multiple chronic conditions have suffered through decades of inadequate social support and uncoordinated care. Their impoverished lives and families too often have been scarred by drugs, alcohol, and physical or emotional abuse. Treatments for their behavioral health problems have been episodic at best, and rarely addressed the underlying causes of their distress. The COVID-19 pandemic has hammered the nation’s low-income communities where these social problems are endemic and exacerbated all the existing problems.
Can attentive care, even delivered consistently over several years, undo a lifetime of neglect?
Their approach now faces its sternest test. Income and wealth inequality, already at an all-time high before the pandemic, is worsening quickly. The government and public’s failure to control COVID-19 U.S. has triggered the worst economic downturn since the Great Depression with unemployment in just four months.
The country is run by an administration that has torn huge holes in the nation’s safety net. Healthcare providers and social service organizations, which cannot plug the gaps in the best of times, face even bigger challenges when demand for food, shelter and social support is rising.
The Challenge for Primary-Care Providers
Giddens, who is disabled, provided a good example of the possibilities and pitfalls of the intensive primary care approach. She benefited from many non-healthcare services under Oak Street’s care. She got free rides to appointments from her subsidized, high-rise apartment. They signed her up for nutrition education and cooking classes.
On the healthcare side, she’s certainly benefited from greater care coordination. Dr. Bhansali put her on insulin instead of metformin since that had failed to control her blood sugar. “A few years ago, my blood sugar was all over the map,” she told me in our initial interview. “Sometimes it got so high, over 600, over 800, it said go to the hospital right away. When I got to Oak Street, that’s when my blood sugar has been normal.”
The month before the pandemic lockdowns began, I checked in with Giddens to see how things were going. Not so well, as it turned out. In May 2019, a series of coughing spells led to renewed seizures, one of which caused her to pass out. She wound up in the hospital. Her doctor ordered her a motorized wheelchair. Last fall, she began vomiting. Three ER visits and multiple invasive diagnostic tests later, she was diagnosed with severe stomach distress from excessive use of naproxen, one of her pain meds.
The idea of lowering costs by targeting patients like Giddens, whose frequent hospitalizations account for a disproportionate share of healthcare spending, first came to prominence in 2011 in an article in The New Yorker. Author Dr. Atul Gawande highlighted the pioneering “hotspotting” work of Dr. Jeffrey Brenner in Camden, N.J.[1] Drawing on data that identified high-
utilizer patients for intensive primary care and additional social services, Brenner’s Camden Coalition launched a pilot project that in 2010 reduced hospital and ER visits by 40%, which reduced spending by 56%.
Gawande acknowledged these savings didn’t include the cost of the program. Nor did they take into account the possibility that patients might have reduced hospital use on their own, what statisticians refer to as reversion to the mean. Yet he concluded that spending under this “strange new approach” was undoubtedly lower and amounted to a “revolutionary” approach in how we care for low-income people with multiple chronic conditions. The article generated enormous buzz in healthcare policy circles and several of Brenner’s acolytes went on to start firms pursuing the strategy.
What the Research Shows
Early in 2020, the movement got its comeuppance when the New England Journal of Medicine published the results of a randomized, controlled trial of the Camden experience over four years. The study suggested the program’s positive results were, in fact, nothing more than reversion to the mean.[2]
The study enrolled 800 patients who had just been hospitalized in Camden. They representated the tough challenges facing
providers in every depressed inner city. Over 80% were impoverished African Americans and Hispanics; a similar percentage was people over 45. More than 90% were on either Medicare or Medicaid. Just 5% were employed; nearly half were substance abusers; and a third suffered from depression.
Half the group enrolled in Brenner’s program, which used nurses, social workers and community health workers to coordinate post-discharge care and link patients to community groups offering social services. The other half got typical discharge instructions and continued to access the healthcare system in their usual manner – whatever that happened to be.
At the end of six months, there was no difference between the two groups on the study’s primary measurement of hospital readmissions. About 62% of both groups had been rehospitalized at least once. “It is possible that approaches to care management that are designed to connect patients with existing resources are insufficient for these complex cases,” the study authors suggested. A companion Perspective in NEJM concluded healthcare policy makers should focus on cost-control efforts an eliminating waste throughout the entire system. “Until somebody jumps into th(at) water, high-cost patients may continue to be high-cost.”[3]
The firms pursuing the intensive primary care strategy rejected the study’s conclusions. They pointed to the five accountable care organizations started in Camden over the four years of the study, suggesting many patients in the control arm may have actually received high-touch care after their discharge from the hospital. They also argued their primary-care programs were better. Less than a third of the people in the intervention arm in Camden visited a primary care physician more than once over the next six months, and few additional people signed up for food stamps.
Intensive primary-care companies also noted that their intensive primary care approach begins earlier than Camden’s. “I am not aware of any organization choosing its patients based on who shows up at the hospital,” said Iyah Romm, CEO of CityBlock. “The goal should be keeping people out of the hospital in the first place.”
CareMore, which has access to claims data through its relationship to Anthem, published a study of its Memphis experience in February 2020.[4] Of the nearly 200 Medicaid patients in the experiment, about a third (71 patients) received CareMore’s intensive primary care program while the other 127 received usual care.
Unlike the Camden experiment, these 71 people had not been hospitalized. Rather, they were high utilizers with multiple chronic conditions whom CareMore’s predictive modeling suggested would continue to be high cost in the coming year. On average they had spent nearly seven days in the hospital and used the ER more than three times in the 12 months before the hospitalization that initiated the study. Their average per-patient, per-year cost was $22,714. Most importantly, CareMore physicians picked all the patients for the randomized as potential beneficiaries of team-based, community-enhanced care.
The experiment ran from March 1, 2017 to February 28, 2018. Over that year, patients given high-touch primary care with social service support reduced their hospital admissions by 44% and bed days by 59% compared to the control arm. Total savings came to $7,732 per member – a one-third reduction in spending.

CareMore officials said their program, unlike Camden, offered a more extensive suite of services. People in the program didn’t visit the CareMore clinic more often than people in the usual care arm of the trial. But they did meet with every member of the CareTeam during their visits. And after each appointment, the community health worker, hired from the community, took on the all-important task of making sure the member got all the necessary transportation, food, housing and other assistance he or she needed.
Another key, CareMore officials said, was getting patients engaged in self-managing their care, which would be impossible without the community health workers who built trust with clients. “Having the community health workers integrated into our primary-care model is a big design difference,” said Dr. Vivek Garg, chief medical officer for CareMore. “The totality of issues these patients face is really tremendous. It’s hard to manage that when you’re caring for someone in your own silo.”
No Magic Bullet
But as Gidden’s experience at Oak Street Health over the past two years suggests, this more intensive approach to caring for complex patients is not a magic bullet. The struggle to keep them on a path toward permanently lower healthcare spending is never-ending. Many of their medical maladies have grown from personal and family histories marred by spotty employment and lifelong poverty, emotional and physical abuse, and physic and physical trauma.
In the two long conversations I had with Giddens, she revealed some of the gut-wrenching events that shaped her life. When a small child, she suffered a severe arm injury after falling out of her crib onto the concrete floor of a Chicago housing project. She never received proper treatment for that injury.
When she was 17, her favorite aunt was murdered by another woman in a jealous rage. Giddens’ father died in 1986 from a rare cancer contracted while working at Sherwin Williams’ Chicago plant, which was fined $5 million a decade later for violating the nation’s environmental laws. Her husband died in 2003 at age 49 after four years on dialysis, a complication of his diabetes. After each trauma, she fell into a deep depression that led either to brief stays in psychiatric facilities or extended treatment with antidepressants.
Throughout her adult life, she worked at low-paying jobs to support her two children: at fast-food establishments, in an airline call center, and, finally, as a casino worker. In 2005, she developed diabetes, a product (she knows now) of a lifelong diet of high-starch, high-fat, fruit-and-vegetable-deficient meals.
Also in 2005, no longer able to stand on her feet all day, she applied for and received permanent disability status, which gave her early access to Medicare. She never found a job that would put to use the business math certificate she’d earned after graduating high school. “I can work up to 9 months and keep my benefits,” she told me hopefully. “As long as it’s something where I sit down, I think I can do it.”
During summer 2020, unemployment is at a post-World War II high. The nation’s poorest communities are suffering the most damage from the COVID-19 pandemic. Even the hope that economic opportunity will make a significant difference in the quality of their lives and health is evaporating. Social support systems like enhanced unemployment benefits and eviction moratoriums are expiring.
The start-up companies and coalitions pursuing the strategy of linking comprehensive primary care to community-based social services are convinced they can make money by taking on the hardest cases in the Medicare and Medicaid portfolio. But unless the U.S. makes a sharp about-face in social policy or votes for change this November, these businesses will face an environment where it will be almost impossible to succeed.
Want to know what healthcare executives are talking about this week? Subscribe to the 4sight Friday RoundUp on iTunes, Spotify, or where ever you listen to podcasts.
Sources
- Atul Gawande, The Hot Spotters: Can we lower medical costs by giving the neediest patients better care?, The New Yorker, January 24, 2011.
- Amy Finkelstein, et al., Health Care Hotspotting – A Randomized, Controlled Trial, New England Journal of Medicine, January 9, 2020.
- J. Michael McWilliams and Aaron L. Schwartz, Focusing on High-Cost Patients — The Key to Addressing High Costs?, New England Journal of Medicine, January 9, 2020.
- Brian W. Powers, et al, Impact of Complex Care Management on Spending and Utilization for High-Need, High-Cost Medicaid Patients, The American Journal of Managed Care, February 2020.





