On Sept. 22, 1962, a young Bob Dylan performed “A Hard Rain’s a-Gonna Fall” for the first time at Carnegie Hall in New York City. Written at the time of the Cuban missile crisis, the iconic question-and-answer song bristles with symbolism and foreboding, anticipating a period of political and social upheaval that would define the decade.
Sixty years later, the nation is embroiled in another period of political and social upheaval, while hospitals have been pushed to the center of the maelstrom by COVID-19 and other forms of industry disruption.
A hard rain will fall on hospitals that fight the strong regulatory headwinds aimed at leveling the competitive playing field for value-based service providers. Apart from COVID-19, the biggest healthcare stories of the past two years have been the adoption and impact of expansive data interoperability and pricing transparency regulations.
Most hospitals haven’t gotten with the program. As evidenced by the AHA’s recent “Cost of Caring” report, too many hospitals prefer to cry poverty and beg for more societal resources.
Responding with More Than Just an Umbrella
Healthcare executives rhapsodize on how free-flowing data exchange will enhance care outcomes, reduce administrative friction, improve customer experience and advance medical research. Yet few hospitals are embracing interoperability. Data systems still don’t talk to each other. They often lack vital patient information.
On payment transparency, most hospitals are paying fines rather than reveal their negotiated treatment rates with commercial health insurers. In response, the Biden administration finalized a new rule last November that increases fines for noncompliant hospitals and prevents hospitals from impeding internet searches through source-code manipulation.
Regulatory pressures on health systems continue to increase. Last July, President Biden issued an Executive Order targeting noncompetitive hospital mergers, surprise billing and price transparency. In October 2021, the Center for Medicare and Medicaid Innovation called for all Medicare beneficiaries to be in risk-based accountable care organizations by 2030.
Overall, the regulatory environment is hostile to hospitals unwilling to embrace change. American society expects more public benefit from nonprofit healthcare than it currently receives. Rather than fight gravity, hospitals must embrace value and consumerism. They must turn those regulatory headwinds into tailwinds.
Leading Change
Darwin’s theory of evolution asserts that a species’ survival depends primarily on its adaptability. Darwinian logic applies to hospitals. Those that adapt business practices that deliver better outcomes at competitive prices with great service will retain market relevance.
Historically, hospitals have been strategically defensive.[1] It’s time to go on offense. It’s time to embrace the new regulatory mandates on transparency, interoperability and anticompetitive behaviors. Healthcare leaders can and should use the new regulations to drive value-based care throughout their organizations.
Proactively disclosing prices will earn consumers’ trust and better position service offerings. Health systems can apply the knowledge they gain from more accurate buy-sell transactions to identify pricing anomalies, stimulate organizational reforms and optimize resource allocation.
This same logic applies to interoperability. By proactively sharing de-identified patient data, hospitals can attract innovative companies to help develop engaging, consumer-friendly digital platforms. Better outcomes, lower costs and superior customer experience will follow.
Finally, hospitals need to curtail anticompetitive behaviors. Far too many use market leverage to negotiate higher prices with commercial health insurance companies. Pursuit of anticompetitive behaviors, including mergers that result in higher treatment prices, is ultimately self defeating. It stymies value creation and inhibits strategic repositioning.
In contrast, hospitals that deliver value-based services do not require anticompetitive tactics to solidify their market positions. Embracing regulatory policies that stimulate transformation is liberating. It frees health systems to concentrate on meeting customers’ vital healthcare and health needs.
Promoting population health is a novel enterprise for most health systems. It requires new payment models, operating behaviors and outcome metrics. Moreover, population health is disruptive to traditional healthcare practices because it reduces the need for acute care treatments.
Implementing conflicting business models is complicated. It requires a form of dual transformation.
Managing Two Business Models Simultaneously
As the healthcare marketplace transitions to value-based care delivery, all hospitals must streamline their transactional healthcare businesses to remain competitive. Some will also undertake community-based population health programs.
Despite requiring the same underlying capabilities, transactional healthcare and population health business models operate in opposition to one another.
In transactional healthcare, higher volume translates into more revenue and profits. Transactional healthcare emphasizes volume and efficiency (per unit care costs).
Meanwhile, population health companies manage care costs within predetermined budgets. Unnecessary volume is a liability. Consequently, they emphasize health promotion, disease prevention, holistic care delivery and disease management to reduce acute interventions and optimize member well-being. Delivering the right care at the right time in the right place creates enormous societal value while aligning provider and patient interests.
As value-based payment models proliferate, transactional healthcare will diminish while population health will increase. Transactional healthcare will not disappear but will assume a commodity focus. Prices for routine services will coalesce at transparent market-based levels.
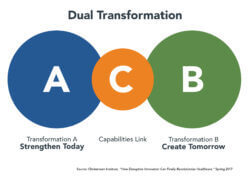
Source: Christensen, C., Waldeck, A., and Fogg, R., How disruptive innovation can finally revolutionize healthcare, Innosight, Spring 2017.
What is required, therefore, is for health systems to adopt a management model called a dual transformation, by which a company can transition its operating profiles during periods of disruptive change.[2] Under this model, a health system can reposition its traditional transactional approach to better adapt to the changing marketplace (depicted as “Transformation A”) while applying the same capabilities (the “C” link) to develop a population health strategy in response to industry innovations and disruptions such as value-based payment (depicted as “Transformation B”).
Dual transformation promotes more efficient operation of traditional businesses, even as they shrink, while nurturing and growing new businesses. There is no overlap in their operations. However, senior management ensures that capabilities flow to both businesses in sufficient measure to optimize organizational success.
The Path to Future Success
Rather than fight regulatory headwinds and the “hard rain” they create, health systems can embrace the new regulatory mandates. After abandoning anticompetitive business practices, health systems can proactively pursue value-based care delivery and community-wide population health. That will put wind in their sails and give them clear skies in their future.






