September 6, 2017
Battling Cancer: Partnering to Make Headway Against Medicine’s Toughest Foe
Medical science has made major advances in treating some cancers (e.g. testicular cancer) by killing or restricting the growth of cancer cells, sometimes curing the disease and otherwise by prolonging life. Other cancers defy treatment and, unfortunately, are often accompanied by a bleak prognosis.
America’s great medical research centers have waged war against cancer for decades. While there is great promise for breakthrough therapies (biologics, hormonal, targeted, genomic) and data-enabled precision medicine, there is limited evidence to date of widespread efficacy.
Consequently, the day-to-day battle to diagnose and treat cancer is primarily tactical and fought in every American community through:
- Prevention
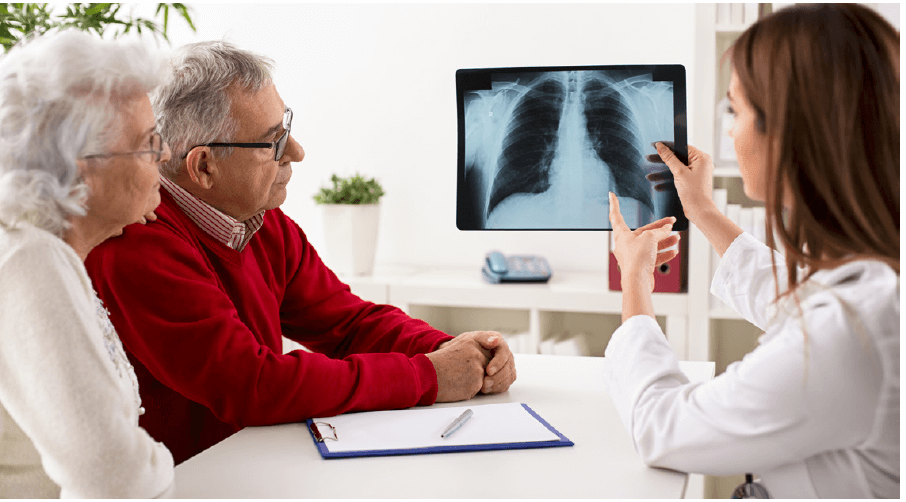
- Better and earlier diagnosis
- Standardized and comprehensive care protocols
- Holistic, patient-centric treatment
- Rigorous follow-up and ongoing monitoring
Almost 40% of Americans will receive a cancer diagnosis during their lifetime.[2] Most cancers are chronic conditions that manifest as people age. Once it strikes, treating cancer is expensive, iterative, prolonged, multi-dimensional and unpredictable.
Organizing and delivering effective cancer care at the community level offers the greatest near-term benefit for extending and enhancing patients’ lives. As with all chronic diseases, meaningful progress against cancer combines evidenced-based treatments with coordinated patient-centric delivery. This requires logistical, technological and organizational expertise.
The Emperor of All Maladies
Dr. Siddhartha Mukherjee’s Pulitzer Prize-winning biography of cancer, “The Emperor of All Maladies” describes cancer’s peculiar malevolence of the disease in vivid terms. Mukherjee wrote, “Down to their innate molecular core, cancer cells are hyperactive, survival-endowed, scrappy, fecund, inventive copies of ourselves.”[4]
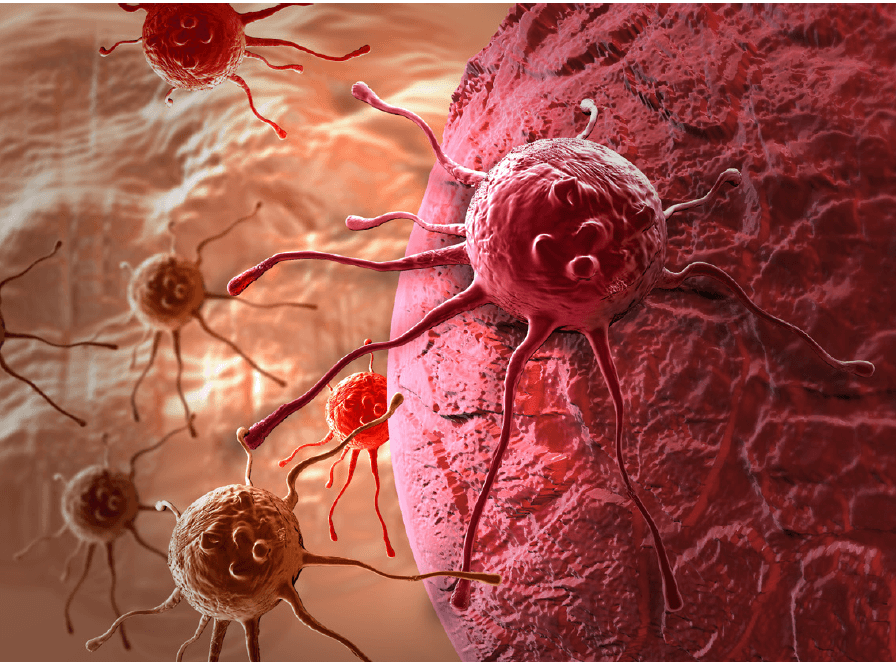
Cancer is easy to define but difficult to treat. Genetic mutations at the molecular level trigger the uncontrolled growth of cells. Cancer cells replicate more quickly than normal cells because they overwhelm the body’s natural barriers against cell growth. Once unleashed, cancer cells attack the body’s organs and the immune system. Few cancers are purely genetic. Almost all cancers have genetic and environmental causal factors.
Over the last 30 years, medical science has begun to understand the biology of cancer at the molecular level. There is great variation in the disease and even within and across tumors. New discoveries often generate as many questions as answers. The “causes” of cancer may be irreducibly complex and impossible to fully understand.
Until medical science cracks cancer’s genetic code, cancer prevention and treatment will continue to emphasize the avoidance of known carcinogens (e.g. tobacco), the adoption of healthy behaviors and the application of proven surgical/medical treatment regimens.
Battling Cancer in the Field
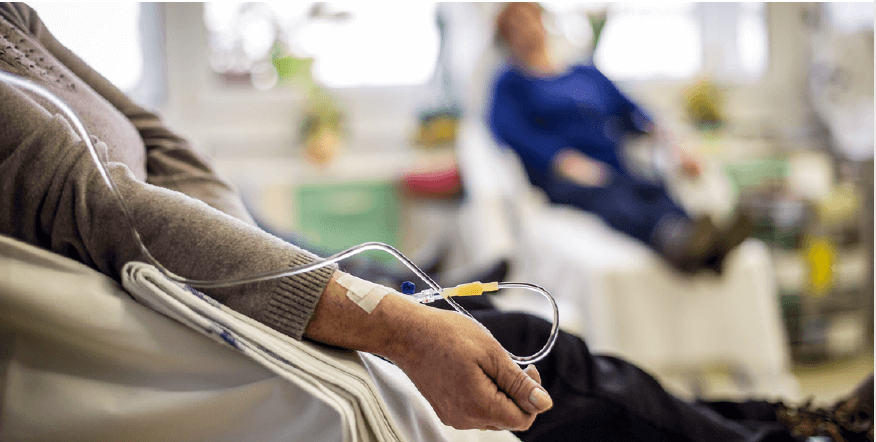
There are two basic approaches to cancer treatment: 1) removing diseased cells; and, 2) limiting their spread and reoccurrence. Much of what we know about effective cancer treatment regimens originates from trial and error medical experiments conducted on countless patients since the late 1800s. Most cancer treatments combine surgery, chemotherapy and/or radiation.
Given America’s enormous investment in clinical research and clinical trials, it’s not surprising that the U.S. leads the world in cancer survival rates. After peaking in 1991 at 215 per 100,000, annual cancer deaths have fallen 23% to 175 per 100,000 even as diagnosis rates continue to rise.[5] This progress results from better screening, earlier diagnoses, more intense and disease-specific treatment regimens and greater access to comprehensive treatment.
While “moonshot” efforts are laudable and genomic breakthroughs earn well-deserved headlines, meaningful progress in improving cancer survival rates has come primarily from better “blocking and tackling” at the community care level.
Up to 90% of cancer care occurs at community centers. Providers are leading the way with better protocols, improved coordination, more patient-centric care delivery and enhanced patient education and engagement.
Cancer Care Delivery: Complex, Costly and Loosely-Coordinated
Cancer care is broad in scope and increasingly comprehensive. Cancer patients receive care from a variety of specialists, technicians, counselors, therapists, and pharmacists. Care occurs in multiple settings, including hospitals, ambulatory facilities, physician offices, physical therapy centers and (increasingly) at home.
There is no national care system in place to organize and coordinate the diverse array of cancer treatment services. Providers organize services in a variety of ways. Cancer care is often fragmented, but that is changing. Some providers, such as Memorial Sloan Kettering Cancer Center, deliver all treatment onsite through owned services. Many operate through coordinated networks of physicians, affiliates and satellite facilities. Here are examples:
- The University of Texas MD Anderson Cancer Center operates satellite sites across Houston where cancer patients can receive chemotherapy, radiation and minor surgery. It also partners with community providers and supports those practitioners with clinical oversight. In 2016, MD Anderson partnered with UnitedHealthcare to test bundled payment arrangements for certain types of cancers, and to coordinate services accordingly. Other cancer centers that deploy community-based services include Dana-Farber Cancer Institute and Mayo Clinic.
- Cancer Treatment Centers of America coordinates care across a national network of five regional hospitals. Using an integrated, patient-centered approach, CTCA assembles a care team for each patient in one location. It deploys care managers to help coordinate and orchestrate care and needed services.
- The U.S. Oncology Network is a network of 1400 affiliated physicians with over 400 locations across the country. The goal is to deliver high quality cancer care at the local level close to where patients live. The Network provides its physicians and practices with business, clinical and practice management support.
Regardless of the setting, cancer care is complex, costly and administratively burdensome. According to the American Society of Clinical Oncology’s 2017 report, “State of Cancer Care in America,” cancer care practices across the country face business, regulatory and operational challenges that absorb time and resources better devoted to patients.
Providers cite overhead and administrative costs as their primary burden. In 2016, they spent an astounding $15.4B and 785 hours per physician to meet reporting requirements alone.[6] Increases in drug prices, especially for new medicines, contributes to rising cancer treatment costs.
e+CancerCare: Platforming Community-Based Cancer Care
Coordinated cancer treatment works. In communities across America, providers are structuring comprehensive cancer care platforms to achieve consistent, high-quality cost-effective outcomes. e+CancerCare illustrates how complementary provider organizations partner to create comprehensive cancer treatment programs.
Founded in 2002, Nashville-based e+CancerCare operates 23 outpatient cancer care service centers in ten states that provide radiation, chemotherapy, imaging, urology, physical therapy and patient counseling in partnership with local providers.
When CEO Tom Weiss joined in 2013, e+ operated as a traditional outpatient service provider. Weiss and his leadership team redefined the company’s mission. Henceforth, e+CancerCare would partner with aligned caregivers in their communities to fight cancer together.
With the benefit of comprehensive treatment services, Weiss believes that “the best place to receive cancer care is in your own community surrounded by a caring team of doctors, nurses, staff, family and friends.”[7] e+CancerCare has the following 4 operating pillars:
- Excellence: Collaborating with physicians to improve the quality of cancer care
- Access: Increasing patient access to comprehensive cancer care
- Empowerment: Developing, supporting and engaging our employees
- Empathy: Treating patients and their families like our own
e+ operates in mid-sized regional cities. The company offers a broad platform of cancer treatment services and capabilities to its provider partners. Together, they deliver coordinated, comprehensive and advanced cancer care.
Scalability, expertise, quality data and experience inform and shape the platform’s service provision. This includes deep knowledge of insurance, coding and compliance requirements. Services are flexible and tailored to meet each provider needs and strategic priorities.
“Our market opportunity,” Weiss says, “is to create platforms that can help physicians and hospitals serve their communities better. We bring management and operational expertise that reduces overhead, improves practice management, navigates patients and ensures complete and efficient compliance, contracting and coding. We don’t take over, we just support providers so they can do what they do exceptionally well.”
Patients love the care. 97% are “very satisfied” with the quality of their physician care. 96% are “very satisfied” with e+’s patient navigator program. 100% reported that all their “non-clinical” needs were met. That’s treating mind, body and spirit.
[2] National Cancer Institute
[3] National Cancer Institute
[4] Siddhartha Mukherjee
[5] American Cancer Society 2016 Fact Sheet
[6] http://ascopubs.org/doi/10.1200/JOP.2016.020743
[7] e+ website
CO-AUTHOR
 Wyatt Ritchie is a senior banker focusing on Post-Acute Care and Outsourced Services. Mr. Ritchie joined Cain Brothers in 2010 with 23 years’ experience advising both public and private companies in a variety of merger and acquisition, capital raising, and strategic advisory transactions. Mr. Ritchie’s recent transactions include the refinancing of senior and subordinated debt for American Surgical Professionals, the sale of Centerre Healthcare to Kindred Healthcare, the sale of Specialty Hospitals of Washington, the recapitalization of Results Physiotherapy by Sterling Partners, and Erickson Living’s acquisition of Devonshire at PGA. He is a member of the Firm’s President’s Advisory Council.
Wyatt Ritchie is a senior banker focusing on Post-Acute Care and Outsourced Services. Mr. Ritchie joined Cain Brothers in 2010 with 23 years’ experience advising both public and private companies in a variety of merger and acquisition, capital raising, and strategic advisory transactions. Mr. Ritchie’s recent transactions include the refinancing of senior and subordinated debt for American Surgical Professionals, the sale of Centerre Healthcare to Kindred Healthcare, the sale of Specialty Hospitals of Washington, the recapitalization of Results Physiotherapy by Sterling Partners, and Erickson Living’s acquisition of Devonshire at PGA. He is a member of the Firm’s President’s Advisory Council.
Prior to joining Cain Brothers, Mr. Ritchie was at Jefferies & Company, responsible for that firm’s healthcare services practice. Prior to joining Jefferies, Mr. Ritchie was at CIBC Oppenheimer for eight years where he was responsible for that firm’s West Coast healthcare services investment banking practice and at Bank of America, where he was responsible for Bank of America’s healthcare leverage finance business.
Disclaimer:
The information contained in this report was obtained from various sources that we believe to be reliable, but we do not guarantee its accuracy or completeness. Additional information is available upon request. The information and opinions contained in this report speak only as of the date of this report and are subject to change without notice. This report has been prepared and circulated for general information only and presents the authors’ views of general market and economic conditions and specific industries and/or sectors. This report is not intended to and does not provide a recommendation with respect to any security. Any discussion of particular topics is not meant to be comprehensive and may be subject to change. This report does not take into account the financial position or particular needs or investment objectives of any individual or entity. The investment strategies, if any, discussed in this report may not be suitable for all investors. This report does not constitute an offer, or a solicitation of an offer to buy or sell any securities or other financial instruments, including any securities mentioned in this report. Nothing in this report constitutes or should be construed to be accounting, tax, investment or legal advice. Neither this report, nor any portions thereof, may be reproduced or redistributed by any person for any purpose without the written consent of Cain Brothers.
Cain Brothers is a member of SIPC. © 2016 Cain Brothers and Company, LLC